Expanding Diabetes Care Beyond the Clinic
Geography and healthcare settings shouldn’t dictate access to quality diabetes care.
Technology has transformed diabetes care for some but not all. We support programs that close the gap between what’s possible and the current reality that too few people are able to receive care from endocrinologists or to use proven tools.
Today’s endocrinologist shortage means the majority of people living with T1D receive diabetes care in a primary care or hospital setting. However, there are community-based, accessible options that can be better utilized. Pharmacists and school nurses are important sources of health information and care. Telehealth providers offer greater access to care, especially specialty care, and more flexibility for people with T1D and their providers. We support efforts to equip community-based providers with knowledge and resources and efforts to realize the full potential of telehealth — to make sure quality T1D care is accessible where people actually receive care.
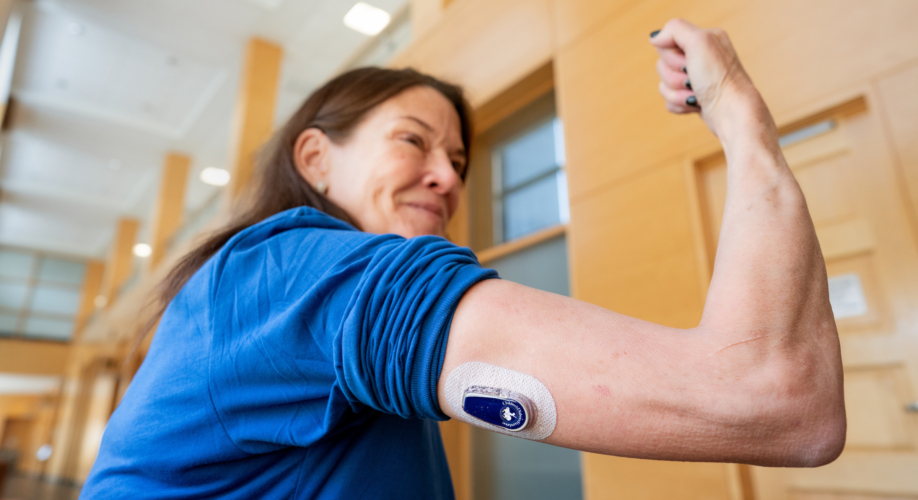
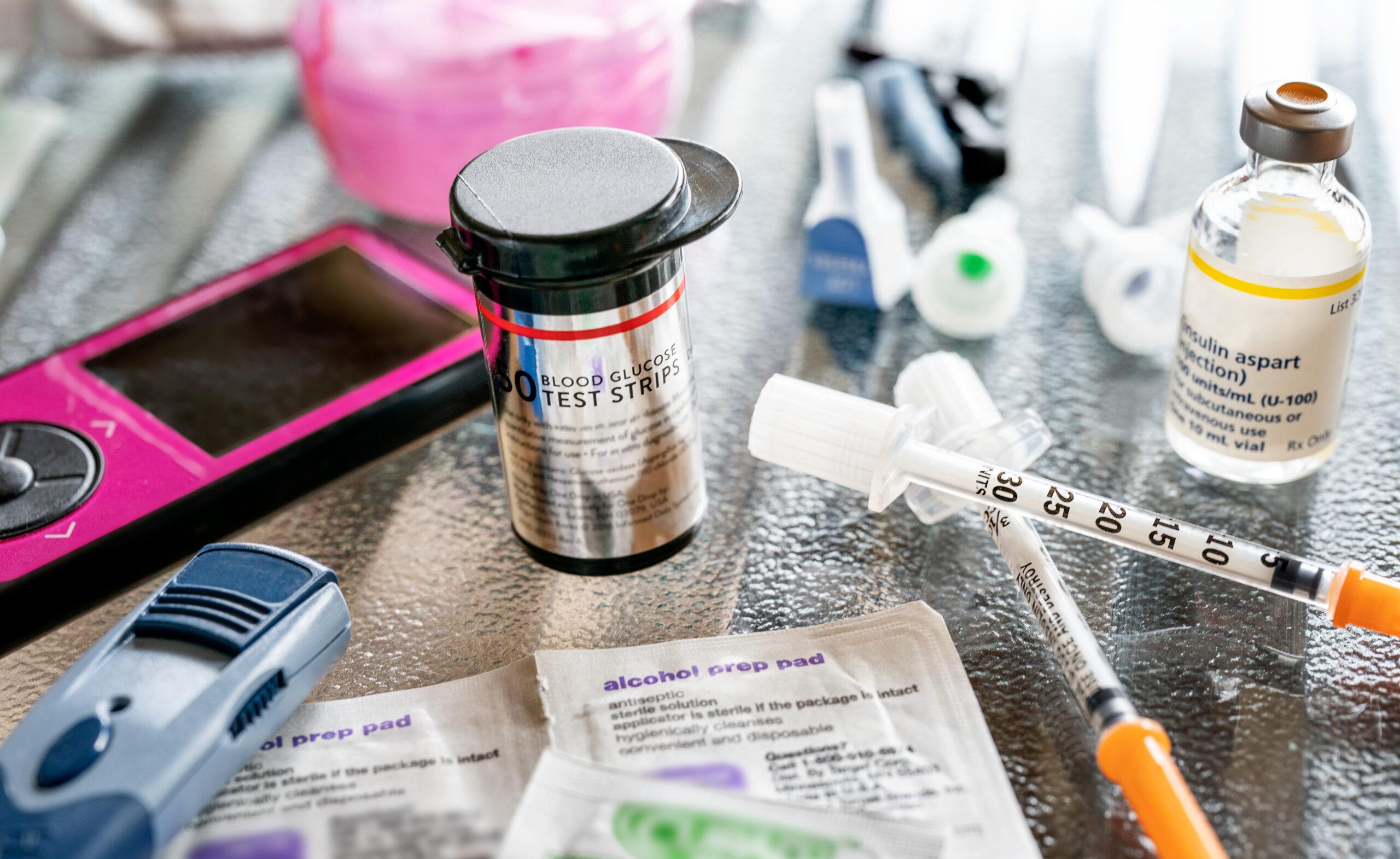
Standard of care for T1D includes utilization of devices such as Continuous Glucose Monitors (CGMs) and Automated Insulin Delivery (AID) Systems, which are proven to improve health outcomes. However, adoption of these technologies is low beyond specialty clinics of endocrinologists. We aim to enable sustained use of these devices by increasing knowledge and access to resources for people and families with T1D, healthcare providers, and other stakeholders.